Rigid bronchoscopy: Tips and Tricks
Melissa Brooks Peterson MD, Myron Yaster MD, and Judit Szolnoki MD
Few emergency procedures can be more terrifying than the emergency removal of a tracheal foreign body in a hypoxemic and decompensating patient, except maybe if the foreign body is a button battery. Today’s Pediatric Anesthesia Article of the Day by Wang et al. discusses anesthesia for pediatric rigid bronchoscopy and is another in a series of pulmonary- and respiration-themed articles in the February issue of the Journal Pediatric Anesthesia. After reading the article I added the book chapter by Vanderhoek et al. from “Smith’s Textbook: Anesthesia for infants and children” because, much to my chagrin, the topic of tracheal foreign body removal was not covered by Wang et al., and I thought it should be. (Smith’s is one of my go to pediatric anesthesia textbooks). I’ve asked Mel Brooks one of the PAAD’s airway experts and commentators and Judit Szolnoki of Nemours Children’s Health system and Mel’s mentor to write this review with me (the other PAAD airway expert, Jamie Peyton, co-authored today’s article) . Finally, this article is accompanied by a podcast that you may be interested in listening to. I’ve included the link. Myron Yaster MD
Original article
Wang JT, Peyton J, Hernandez MR. Anesthesia for pediatric rigid bronchoscopy and related airway surgery: Tips and tricks. Pediatr Anesth. 2022 Feb;32(2):302-311. PMID: 34877742
Accompanying podcast:
https://pediatricpods4.podbean.com/e/anesthesia-for-pediatric-rigid-bronchoscopy-and-related-airway-surgery-tips-and-tricks-january-2022/
Book chapter
Vanderhoek SM, Dalesio NM, Schwengel DA: Anesthesia for Otorhinolaryngologic surgery. Smith’s Anesthesia for infants and children, 10th edition. Editors: Davis PJ and Cladis FP. Elsevier, Philadelphia PA, 2022
The Wang et al article focuses on these topics: Dynamic 3-phase rigid bronchoscopy used to evaluate tracheomalacia, bronchoscopy for open airway surgeries, such as suspension laryngoscopy procedures, rigid bronchoscopy under direct laryngoscopy and aerodigestive combined procedures, and rigid bronchoscopy for TEF occlusion and tracheal/open-airway surgery. Obviously, the book chapter is more exhaustive and encyclopedic and discusses everything from anesthesia for T&A surgery, to laser surgery, to foreign body removal.
To get to the meat of our discussion: Because we are sharing the airway with our surgical colleagues, “the anesthetic management of children with airway diseases is a complex endeavor that requires constant communication with the procedural team, understanding of the surgical procedures, and skill in adapting anesthetic technique to each unique situation.”(1). In our opinion, and in full agreement with our colleagues, communication is the most critical portion of anesthetic care during the open airway and rigid bronchoscopic procedures. This is not an anesthetic that is appropriate for the “blood brain barrier” (the ether screen/drape division) or any “them/us” thinking; rather, nimble adaptation and clear communication is paramount. In my (MBP) practice, I lever the use of closed-loop communication, teach our trainees to utilize this communication exclusively, and I am grateful that my ENT and pulmonary colleagues do the same.
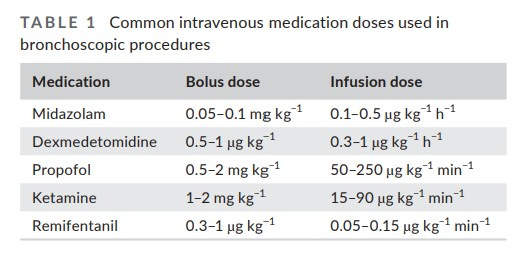
A recurrent theme throughout these sources of information is how to balance the need for spontaneous ventilation and yet maintain an adequate depth of anesthesia to insure immobility and minimal-to-no response to the profound surgical stimulation of the rigid bronchoscope. After induction of anesthesia, TIVA is the most common anesthetic technique for both ease of titration and to minimize room pollution from anesthetic gasses. Both Wang et al and Vanderhoek et al recommend some combination of propofol plus remifentanil and/or dexmedetomidine. Other supplemental drugs include ketamine and midazolam and an anti-sialagogue such as glycopyrrolate (or atropine). We’ve copied table 1 from Wang et al. to provide the common TIVA doses recommended in today’s PAAD.
We want to share with you some take away thoughts regarding anesthetic medication choices for rigid bronchoscopy: I (MBP) take a different tack with medication choices for rigid bronchoscopy – I design the anesthetic to be predictable, short-acting, and to have minimal side effects. As a means to this end, I agree with the authors that the use of IV and/or topical lidocaine to diminish airway reactivity and to reduce the cough reflex is always a good idea (with the exception of allergy). I avoid anything long-acting as one way or another these children have some level of airway compromise that will be still present postoperatively. I recommend designing the anesthetic to have the patient wide awake as soon as possible after the case to minimize sedation, minimize atelectasis, minimize the need for supplemental oxygen and to optimize respiratory mechanics in the PACU -- and therefore have an immediate assessment of the patient’s respiratory status. This method has the added benefit of maximizing your chances of an outpatient disposition. While tempting, we don’t think ketamine is a good choice for these procedures due to secretion production – and our ENT and PACU colleagues notice it. Secretions are the enemy in an open airway!
Further, low-dose fentanyl will achieve a balanced anesthetic to avoid huge doses of propofol and provide analgesia from the stimulation of the rigid bronchoscopy. The upside of fentanyl is that it’s short-acting and has an analgesic effect that provides for a nice, prompt wake up in phase 1 PACU with good pain control. Remifentanil can cause unexpected apnea due to its potency in case of an inadvertent bolus due to changing the rate of IV fluid administration and can also be somewhat abrupt in its offset; even with carefully titrated dosing, so buyer beware. It is also extremely expensive compared to fentanyl. No matter which opioid, a low-dose, short-acting opioid is a great adjunct for rigid bronchoscopy and must be appropriately titrated by a knowledgeable pediatric anesthesiologist.
Another critical consideration is avoidance of a prolonged PACU stay and prolonged sedation/prolonged emergence following the procedure – which can contribute to increased atelectasis, oxygen requirement in PACU, unexpected admission. Thus, I (MBP) reserve dexmedetomidine only when absolutely needed, (e.g. for patients with severe OSA in whom opioids cause prolonged apnea, or for patients having an airway surgical intervention who are going to be admitted post-procedure, and prolonged sedation will not delay their PACU care).
Common features of the anesthetic techniques for this diverse group of procedures is how to balance the need for spontaneous breathing, even coughing on purpose! (a dynamic tracheal evaluation) versus assessment of the airway under fixed conditions (no coughing, minimal breathing or even controlled ventilation) and how to prevent hypoxemia during these procedures.
Preventing intraoperative hypoxemia is the other unifying theme of these articles and is best accomplished by always providing supplemental oxygen during the procedure either by attaching oxygen (green tubing) directly to the side port of the rigid bronchoscope, through the anesthesia machine via a small caliber endotracheal tube held by the surgeon in the corner of the patient’s mouth or attached to a 6 tracheal tube directly attached to the side port of the bronchoscope. Alternatively, and we would argue the future of routine airway management, supplemental oxygen can be provided via high flow nasal cannula/HFNC (thank you to our friends in Perth, namely Dr. Von Ungern-Sternberg, for studying and popularizing this technique!) (2)
Although not a key point of the article, I (MBP) want to expand on the anesthetic management of children with aerodigestive disorders because it is a special interest of mine. These children “frequently present with a constellation of related comorbidities that affect feeding, swallowing, breathing, and airway integrity. Presenting symptoms often include stridor, chronic cough, recurrent aspiration, dysphagia, recurrent pulmonary infections, either in isolation or in concert. Due to the inter-related nature of the disease processes, there has been increasing interest in developing multidisciplinary complex care teams comprised of members from the specialties of otorhinolaryngology (ORL), pulmonology, gastroenterology (GI), and anesthesiology to streamline the diagnostic work-up process and improve outcomes. Studies have shown the combined procedures can decrease total anesthesia time, decrease cost, and improve family satisfaction from decreased wait time and fewer hospital visits.”(1,3) The provision of anesthesia for aerodigestive evaluations (“the triple scope”) is a mash-up of all of the above techniques described, and requires the nimble adaptation, closed-loop communication, a clear and purposeful anesthetic plan with intentional medication choices, and a willingness to achieve 3 different types of anesthesia in a single 45-minute case. In our opinion, it is “L’ Apogeé” of all of the challenges the authors of the article and book chapter touch on.
Finally, the management of foreign body aspiration is very similar to the management of the triple scope in aerodigestive patients, with the added challenge of a child who can be profoundly ill depending on the nature, timing, and location of the foreign body. Most commonly mask induction is followed by spontaneous ventilation using a combination of topical and IV lidocaine, propofol TIVA, judiciously titrated short-acting opioids, and possibly sevoflurane. Positive pressure should be avoided but can be used as an intermittent rescue or “oh shit” strategy, as it may change the position of the foreign body and prolong the time it takes to extract it. Of course, we cannot end this PAAD without reminding ourselves that a smooth, nimble, controlled, spontaneously breathing, non-coughing general anesthetic is critical to avoid the most feared complication of foreign body removal: complete obstruction or loss of the airway; never forget that ECMO may be your end game in the worst of scenarios – keep it in your back pocket!
Melissa Brooks Peterson MD, Myron Yaster MD, and Judit Szolnoki MD
References
1. Wang JT, Peyton J, Hernandez MR. Anesthesia for pediatric rigid bronchoscopy and related airway surgery: Tips and tricks. Paediatr Anaesth 2022;32:302-11.
2. Humphreys S, von Ungern-Sternberg BS, Skowno J, Williams T, Taylor J, Taverner F, Gibbons K, Burgoyne L, Sommerfield D, Stephens P, Hallett B, Vijayasekaran S, Slee N, Burns H, Sowa M, Davidson A, Schibler A. High-flow oxygen for children's airway surgery: randomised controlled trial protocol (HAMSTER). BMJ Open 2019;9:e031873.
3. Ruiz AG, Bhatt JM, DeBoer EM, Friedlander J, Janosy N, Peterson MB, Wine T, Deterding R, Prager JD. Demonstrating the benefits of a multidisciplinary aerodigestive program. Laryngoscope 2020;130:521-5.