Preventing wrong sided blocks
Myron Yaster MD, Eugenie S. Heitmiller MD, and Jayant K. Deshpande MD
Today’s PAAD by Ha1 opens with the following statement: “Forty-five percent of medical errors occur in the operating room,2 and wrong-site procedures remain one of the most preventable medical errors3.” Really? 45% of ALL medical errors occur in the OR? I can’t believe that statement but whether it is true or not, a wrong sided procedure whether by a surgeon or anesthesiologist is a “never event”, that is, should never happen.4 What are never events? They are invasive procedures performed in any patient care setting on the wrong part of the body, the wrong side, or in the wrong patient, and which exposes the patient to more than minimal risk.”1 Today’s PAAD reviews the causes of wrong-sided nerve blocks and offers potential solutions to decrease the risk of this never event from happening.
By the way, today’s PAAD is another safety article from the current volume of the International Anesthesiology Clinics. We’ve already reviewed a couple of articles from this issue and expect to see more articles from this journal in the days ahead. Myron Yaster MD
Original article
Ha J. Preventing wrong-sided blocks. Int Anesthesiol Clin. 2024 Apr 1;62(2):53-57. doi: 10.1097/AIA.0000000000000436. Epub 2024 Feb 26. PMID: 38404146
“Wrong-site errors commonly involve symmetrical structures, and, therefore, are usually wrong-sided errors.5 The most frequently involved specialties noted for wrong-site errors are orthopedic surgery (22.4%), general surgery (16.8%), and anesthesiology (12.1%).6 Wrong Sided Surgery (WSS) is a serious reportable sentinel event and is labeled by the National Quality Forum as a “never event”,4 i.e., something which should never occur and are not a medical risk the patient must accept or be exposed to.5”1
OK, this sounds pretty reasonable, but are wrong sided blocks a real problem? The good news is that regional anesthesia and peripheral nerve blocks have transformed the practice of pediatric anesthesiology and continues to increase in our everyday practices.7 The bad news is that as the number of blocks increases so does the risk and number of wrong sided nerve blocks (WSNBs) increases as well.8,9 Indeed, “a systematic literature review of 70 publications addressing WSNBs by Deutsch et al provides a rate of 0.52 to 5.07 per 10,000 blocks.9”1 Thus, this is a real problem and begs the question, “is there anything we can do about it?”
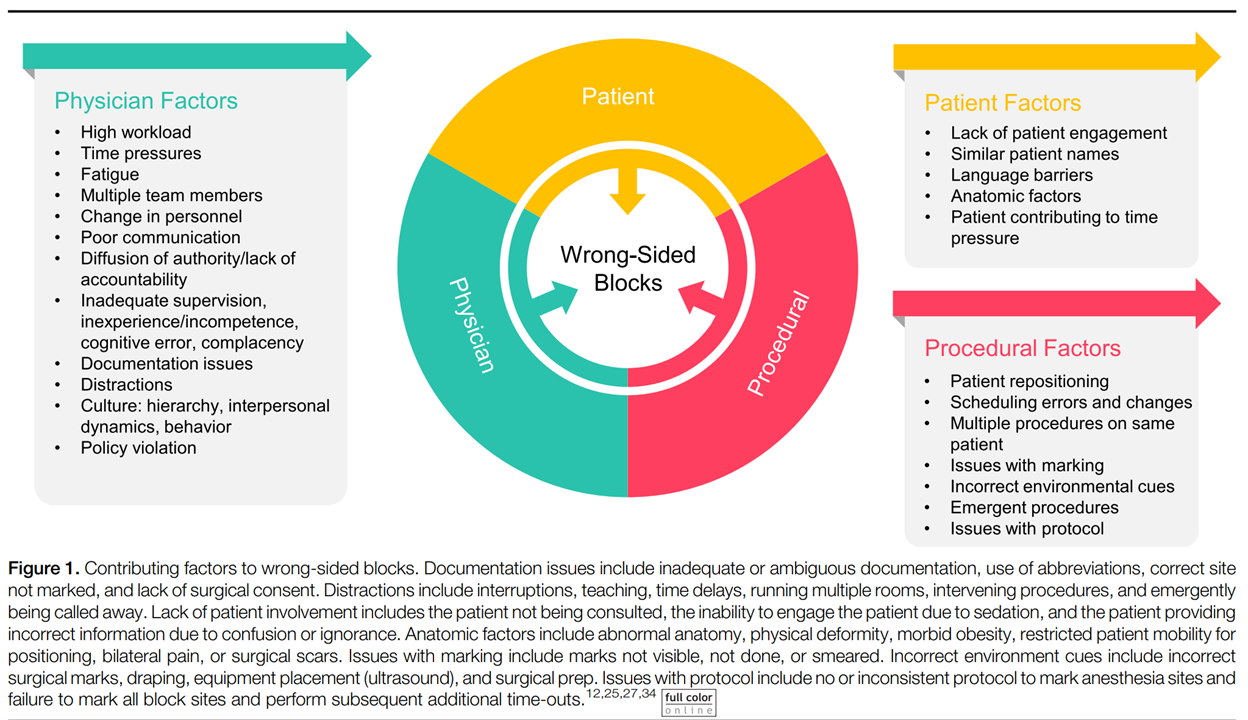
Of course! Ha breaks down the major contributing factors to WSNBs “into categories of procedural-, physician, and patient-related factors in Figure 1”1 and how each can be attacked.
A recurrent theme from the current volume of the International Anesthesiology Clinics and highlighted again in today’s PAAD is the value of checklists and the mandatory use of the Joint Commission’s Universal Protocol. The Joint Commission Universal Protocol applies to surgical and invasive procedures that expose patients to more than minimal risk. It consists of 3 steps: conducting a preprocedure verification process, marking the procedure site, and performing a time-out.10
As discussed in previous PAADs, “A checklist is an inexpensive, simple tool that can help to improve communication and teamwork and reduce variability and error in other complex, interconnected systems.” “Vacheron et al.11 have specifically suggested using a checklist before beginning a block (“stop before you block”), posting warnings in the form of posters or stickers, using physical barriers (e.g., placing a reminder on the ultrasound apparatus), or through a “mock before you block” procedure that requires patient participation.”1 An example of regional block time out from Ha’s article is reproduced below.
Ha concludes: “Wrong-sided blocks are rarely the result of any single factor. Errors often occur in the context of complex clinical situations that increase clinicians’ workload, decision-making under stress, and poor coordination among team members. Any clinician who performs regional anesthesia must be aware of the risk factors for WSNBs and exercise vigilance when multiple risk factors may be present.”1
Have you introduced a formal time out and checklist (stop before you block) in your practice? What tips can you provide to our readers to support its use? What roadblocks did you have to overcome to change practice? Do you review and audit near misses in your M&Ms and safety reviews? Send your thoughts and comments to Myron who will post in a Friday Reader Response.
References
1. Ha J. Preventing wrong-sided blocks. International anesthesiology clinics 2024;62(2):53-57. (In eng). DOI: 10.1097/aia.0000000000000436.
2. O'Connor T, Papanikolaou V, Keogh I. Safe surgery, the human factors approach. The surgeon : journal of the Royal Colleges of Surgeons of Edinburgh and Ireland 2010;8(2):93-5. (In eng). DOI: 10.1016/j.surge.2009.10.004.
3. Al-Nasser B. Unintentional side error for continuous sciatic nerve block at the popliteal fossa. Acta anaesthesiologica Belgica 2011;62(4):213-5. (In eng).
4. Treadwell JR, Lucas S, Tsou AY. Surgical checklists: a systematic review of impacts and implementation. BMJ quality & safety 2014;23(4):299-318. (In eng). DOI: 10.1136/bmjqs-2012-001797.
5. Clarke JR, Johnston J, Finley ED. Getting surgery right. Annals of surgery 2007;246(3):395-403, discussion 403-5. (In eng). DOI: 10.1097/SLA.0b013e3181469987.
6. Stahel PF, Sabel AL, Victoroff MS, et al. Wrong-site and wrong-patient procedures in the universal protocol era: analysis of a prospective database of physician self-reported occurrences. Archives of surgery (Chicago, Ill : 1960) 2010;145(10):978-84. (In eng). DOI: 10.1001/archsurg.2010.185.
7. Handlogten K. Pediatric regional anesthesiology: a narrative review and update on outcome-based advances. International anesthesiology clinics 2024;62(1):69-78. (In eng). DOI: 10.1097/aia.0000000000000421.
8. Nixon HC, Wheeler P. Wrong-site lower extremity peripheral nerve block: process changes to improve patient safety. International anesthesiology clinics 2011;49(2):116-24. (In eng). DOI: 10.1097/AIA.0b013e3181ffc03f.
9. Deutsch ES, Yonash RA, Martin DE, Atkins JH, Arnold TV, Hunt CM. Wrong-site nerve blocks: A systematic literature review to guide principles for prevention. Journal of clinical anesthesia 2018;46:101-111. (In eng). DOI: 10.1016/j.jclinane.2017.12.008.
10. Angle JF, Nemcek AA, Jr., Cohen AM, et al. Quality improvement guidelines for preventing wrong site, wrong procedure, and wrong person errors: application of the joint commission "universal protocol for preventing wrong site, wrong procedure, wrong person surgery" to the practice of interventional radiology. Journal of vascular and interventional radiology : JVIR 2009;20(7 Suppl):S256-62. (In eng). DOI: 10.1016/j.jvir.2009.04.023.
11. Vacheron CH, Acker A, Autran M, et al. Insurance Claims for Wrong-Side, Wrong-Organ, Wrong-Procedure, or Wrong-Person Surgical Errors: A Retrospective Study for 10 Years. Journal of patient safety 2023;19(1):e13-e17. (In eng). DOI: 10.1097/pts.0000000000001080.