Pain in the PICU: Does it affect quality of life after discharge?
Myron Yaster MD, Lynne Maxwell MD, Justin L. Lockman MD, MSEd
Original article
Mallory B Smith, Elizabeth Y Killien, Leslie A Dervan, Frederick P Rivara, Noel S Weiss, Robert Scott Watson. The association of severe pain experienced in the pediatric intensive care unit and postdischarge health-related quality of life: A retrospective cohort study. Paediatr Anaesth. 2022 Aug;32(8):899-906. PMID: 35426458
Pediatric patients admitted to the PICU commonly experience pain either from underlying disease states, the after-effects of surgery/trauma, or from painful procedures that commonly occur in the PICU. Over the years, we have seen the pendulum swing from “babies can’t/don’t feel pain” to general anesthesia for all intubated patients, and back towards progressive mobility (a la. Sapna Kudchadkar and PICU Up! https://www.johnshopkinssolutions.com/solution/amp/picu-up/). But does pain experienced by children in the PICU affect their post-discharge health-related quality of life (HRQL)? Dr. Jennifer Rabbitts1,2 whose research focuses on the long-term effects of pain and sleep deficiency on health outcomes, the development of chronic pain following surgery, and prescription opioid misuse, is the Director of the Center for Clinical and Translational Research at Seattle Children’s Hospital. In case you missed it, she gave great presentations on these topics at recent SPA and SPPM meetings. Based on her findings, it isn’t surprising that in today’s PAAD, Dr. Mallory Smith et al3 (also from at Seattle Children’s Hospital) found, in this retrospective cohort study of medical and surgical patients, that PICU patients with severe pain (pain scores > 7 for > 25% of pain scores in a day) had lower HRQL scores after discharge than those who didn’t.
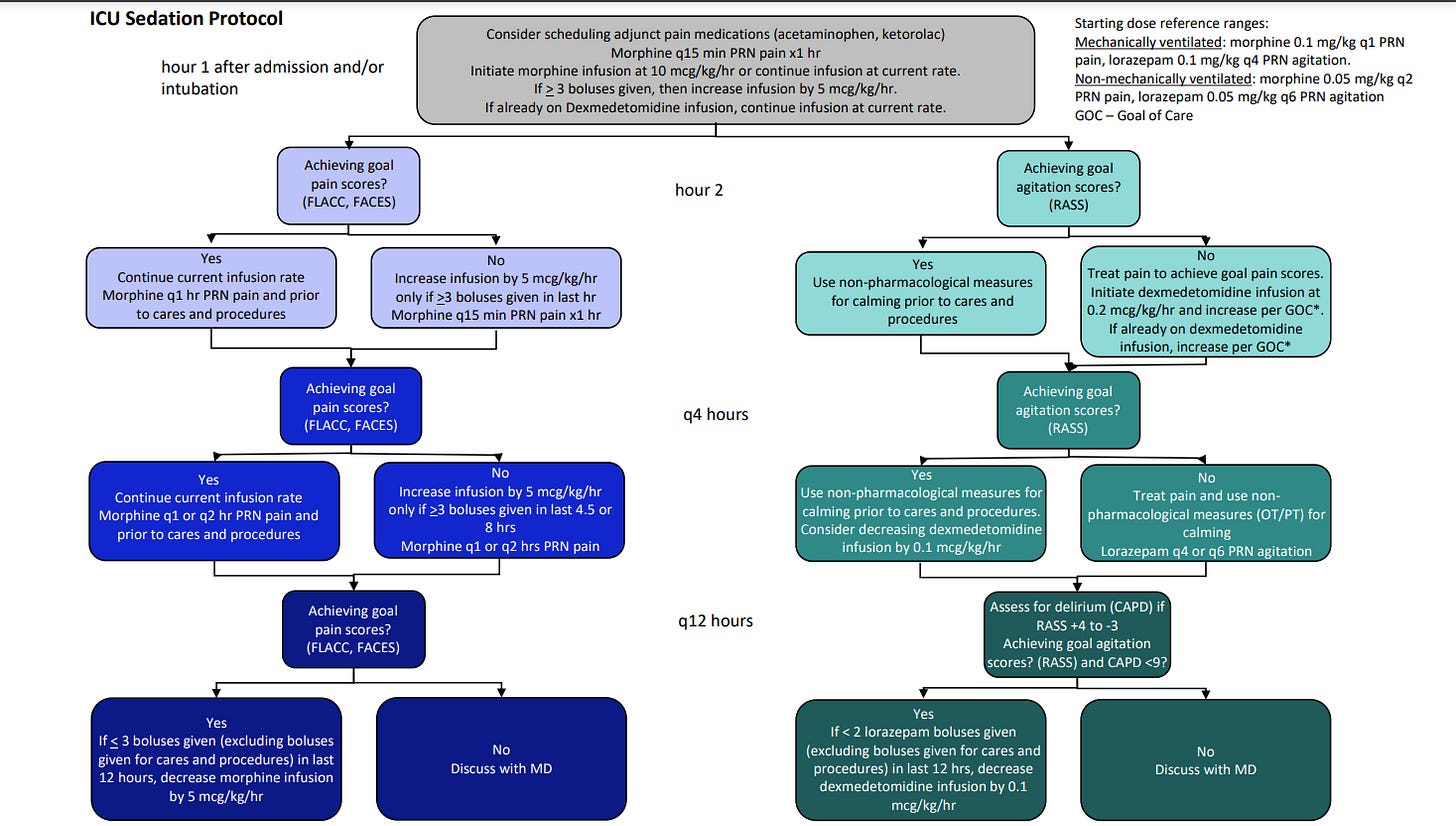
In this study, PICU pain and sedation management was guided by a nurse-led protocol (figure). The standard management included a continuous opioid infusion and dexmedetomidine in addition to acetaminophen and ibuprofen for patients without contraindications to these medications (figure, from digital Supplement 1).3 Lorazepam and neuromuscular blockade were also allowed, but their use was not specifically delineated in the protocol. Pain scores were either nurse- or patient-reported, depending on whether patients could self-report (e.g., influenced by age or neuromuscular blockade),
Not surprisingly, HRQL scores declined in a linear pattern for each additional day of severe pain, more so for surgical than medical patients. “Additionally, patients with severe pain had longer hospital LOS than patients without severe pain, despite having similar severity of illness and baseline health status. In these patients, side effects from the higher opioid doses patients with pain received, medication weaning time, or other clinical factors may have contributed to longer hospitalizations.”3
Again not surprisingly, children with more severe pain more often developed chronic pain and had more problems with sleep, anger and behavioral difficulties akin to those experiencing post-traumatic stress disorders.4 Not discussed is the role of anesthetic management in the surgical patients. Did the surgical patients receive intraoperative opioids and if so which ones and how much? Seattle Children’s is a leader in opioid-free or sparing anesthesia and post-anesthetic care in the outpatient setting. I (MY) wonder, could this have carried over to the inpatients and been partially responsible for the increased pain and the need for more opioids in this study? Or were high doses of intraoperative opioids responsible for hyperalgesia? It would be valuable to present and analyze these data as well.
The authors note a few important limitations, including but not limited to being a single center study, the lack of data about patient coping/support mechanisms and resiliency factors, and the risk of recall bias from the HRQL assessment which was done by parental proxy.
Finally, the authors suggest a greater role for multi-modal analgesia, particularly, regional anesthesia to reduce pain in PICU patients. We couldn’t agree more, and overall think that ICUs benefit from collaborative relationships with regional anesthesia, child life specialists, music therapy, and other experts for optimal patient care. However, I (MY) can’t help but wonder why patients in this protocol had severe, persistent pain. Could the use of IV patient, nurse, and/or parent controlled opioid PCA have provided improved analgesia that was clearly insufficient in this study? What do you think?
References
1. Rabbitts JA, Palermo TM, Zhou C, Mangione-Smith R: Pain and Health-Related Quality of Life After Pediatric Inpatient Surgery. J Pain 2015; 16: 1334-1341
2. Rabbitts JA, Fisher E, Rosenbloom BN, Palermo TM: Prevalence and Predictors of Chronic Postsurgical Pain in Children: A Systematic Review and Meta-Analysis. J Pain 2017; 18: 605-614
3. Smith MB, Killien EY, Dervan LA, Rivara FP, Weiss NS, Watson RS: The association of severe pain experienced in the pediatric intensive care unit and postdischarge health-related quality of life: A retrospective cohort study. Paediatr Anaesth 2022; 32: 899-906
4. Aspesberro F, Mangione-Smith R, Zimmerman JJ: Health-related quality of life following pediatric critical illness. Intensive Care Med 2015; 41: 1235-46