Error traps in the intrahospital transport of critically ill and anesthetized children
Maureen Banigan MD MS, Shyam Deshpande MD, Myron Yaster MD, and Justin L Lockman MD MSEd
“A trap is only a trap if you don’t know about it. If you know about it, it’s a challenge.” - China Miéville
I remember a surgery fellow once breathing a sigh of relief at the end of a long-complicated bowel resection in a 2.5 kg premature neonate saying “aren’t you so glad that’s over?” as the drapes came down. I quipped back, “I won’t be glad until I’m walking out of the NICU with my med box!” After all, the most difficult part of the case was just starting: leaving the homefield safety of the heated OR and my nearby colleagues to transport a medically-complex premie who had just had a major change in his thoracoabdominal compliance and had ongoing third-spacing of fluids through the wild west of the hospital hallways… Talk about a challenge!
Intrahospital transport is an everyday event for anesthesiologists, but it is far from routine. Indeed, there are many potential safety events just waiting to happen1, and the incidence of adverse events may approach 80% 2, with as many as 9% of patients requiring medical intervention.3,4 Importantly, Haydar and colleagues have previously found that nearly 60% of pediatric transport-related events were potentially preventable.5 This is one of the reasons why the frequency of bedside surgery in the neonatal ICU has increased in recent years at many centers.
Known risk factors for complications during transport can be broadly classified as patient-specific (higher severity of illness, younger age, need for mechanical ventilation or vasoactive infusions), equipment-related (use of transport ventilators and monitors) or situational (longer duration of transport, poor hand-off communication, emergency transport, less experienced personnel). Today’s PAAD, also by Dr. Bishr Haydar, highlights some of the error traps of transporting critically ill children and is yet another in the error trap series published in the journal Pediatric Anesthesia. I’ve asked 3 of CHOP’s dual trained anesthesiologist-intensivists to author this review with me. Myron Yaster, MD.
ORIGINAL ARTICLE
Haydar B. Error Traps in the Intrahospital Transport of Critically Ill and Anesthetized Children. Paediatr Anaesth. 2025 Jul;35(7):497-503. doi: 10.1111/pan.15112. Epub 2025 Apr 8. PMID: 40198097; PMCID: PMC12149488.
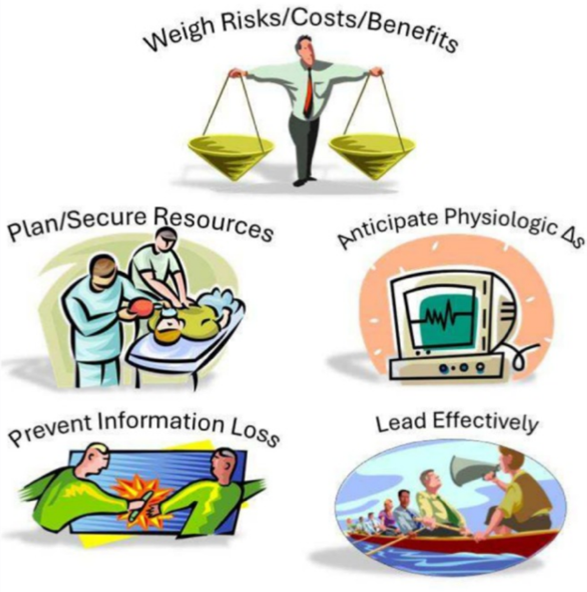
Error traps describe the combination of circumstances and human cognitive limitations that lead to avoidable harm if unmitigated.6 In the article today, Dr. Haydar not only identifies common error traps (see figure) that can occur in intrahospital transport, but also highlights individual- and systems-level countermeasures which provide a foundation for improving perioperative practice. We urge you to consider reading the entire article in its entirety; we will highlight a few of the key points but really cannot do this great article justice without reprinting the whole thing!
ERROR TRAP #1: Failure to Fully Weigh All Risks, Costs, and Benefits Associated With Transport for a Procedure or Test
Before undertaking any critical transport, we should ideally pause and make the space for a multidisciplinary discussion between the anesthesiologist, intensivist, and the proceduralist/surgeon. We each have different skillsets, and (particularly in unstable patients and/or those receiving advanced physiologic support) sometimes moving the patient is not the best option. Questions that should be addressed include: “Is it safe (or even possible) to transport?”, “Is a bedside alternative available?”, and “What are the risks of transport and unique vulnerabilities for this patient?” Involving interdisciplinary team members (e.g., nursing and respiratory therapy) can reveal subtle or nuanced patient issues/risks that may not be apparent by review of the chart alone. If, despite the risks, the patient’s survival is dependent on transport, it is ideal to “optimize procedural timing, typically during normal business hours.”
Although not discussed in the article, it is our impression that anesthesia is now so “apparently safe” that many colleagues do not even consider the risks of anesthesia, let alone transport, when considering procedures. It is our job as anesthesiologists to serve as transport team leaders and the first line of defense against transport-related adverse events. It is also essential to have (and document) a frank discussion with both the entire care and the patient/family if we believe transport or the planned procedure carries a high likelihood of medical deterioration or death. And because critically ill children by definition have dynamic, evolving physiologic perturbations, transports often merit reevaluation/reassessment immediately prior to any physical movement.
ERROR TRAP #2: Failure to Secure Appropriate Resources for Transport and at Every Destination
In the words of Benjamin Franklin, “An ounce of prevention is worth a pound of cure.” Anticipation of clinical deterioration and preparation of appropriate personnel, equipment, and monitoring are crucial. Transport teams should include personnel with expertise in managing all required equipment (e.g., a perfusionist for patients requiring ventricular assist devices (VADs) or on ECMO. Dr. Haydar emphasizes that while the attending anesthesiologist may feel comfortable operating certain devices, this is not advisable during high-risk transports. The anesthesiologist should be available to manage the team and to direct overall care, akin to any team leader. Along those lines, it is crucial to identify roles/responsibilities prior to transport so that each transport task is managed and role are predetermined in the event of emergency. We should not hesitate to ask for additional personnel if needed.
Medications necessary for resuscitation should be readily available and equipment should be fully charged and capable of functioning for the entirety of the transport duration. USE A CHECKLIST! If you don’t have one, now is the time to develop one – sample checklists are conveniently provided in the article. A key step in transport is to untangle the wires, tubes, and infusions. SIMPLIFY, SIMPLIFY, SIMPLIFY! Additionally, it is vital to ensure the destination site is operational and ready to receive the patient – for transport in both directions.
ERROR TRAP #3: Failure to Provide Pertinent Information During Transfers of Care
Handoffs are high-risk times with regards to patient safety and lost information, and intrahospital transports almost always involve handoffs. Handoffs often occur in dynamic environments where the patient status is changing and team members are both multitasking and unknown to each other. “Information loss during these handovers have resulted in double or missed doses of antibiotics and antiepileptic drugs and loss of critical information regarding patient status, resulting in serious errors and potential harm.”1,7 Standardization of post-operative handoffs via checklists improve information exchange and patient outcomes in pediatric cardiac populations (and we suspect others).8 Dr. Haydar suggests that ideally pre-transport team communication should resemble the more familiar interprofessional post-operative handoff. Checklists can help, as can explicitly asking the intensivist to identify the most likely mode of decompensation. This should all be part of the pre-transport discussion as discussed above.
ERROR TRAP #4: Failure to Anticipate Physical and Physiological Changes Associated with Transport
Dr. Haydar highlights three categories of changes to anticipate during transport: changes in equipment, changes in patient position, and physiologic effects of medications administered to facilitate transport. For mechanically ventilated patients, we must decide whether to continue an ICU ventilator, transition to a portable ventilator, or hand ventilate. Transport ventilators often have different circuit compliance and apparatus dead space, which can result in inadequate ventilation (especially in neonates and/or patients with poor lung compliance) even on the same apparent settings. Of 86 cardiac arrests during transport in the Wake-Up Safe database, 58.1% had respiratory causes with 21.4% occurring during preoperative transport and 75.5% post-operatively.5 If device or mode of ventilation is changed for transport, patient stability on that device should ideally be demonstrated prior to movement. Also, verify that disconnect and high airway pressure alarms are enabled, and confirm oxygen reserves and battery supply. (Remember, and this is a frequent Board exam question, a full tank of oxygen has approximately 650 L/oxygen when the pressure gauge reads 2,200 pounds per square inch) Patients on continuous renal replacement therapy will need to be disconnected prior to transport, while patients with VADs or on ECMO will require appropriate backup equipment.
Changes in patient position or just changing bed surface) to facilitate surgical procedures or diagnostic imaging can result in malpositioned or kinked endotracheal tubes or other drains, unplanned extubation, dislodged vascular access or inadvertent disconnection of infusions. Physical movement can cause significant pain or stimulus with subsequent alterations in respiratory compliance and venous return, which can be deleterious in patients with pulmonary hypertension or increased intracranial pressure. For this reason, sedative and/or neuromuscular blocking agents are often given in preparation for transport to reduce the risk of complications, but for some patients may lead to difficulty ventilating or hemodynamic instability. As noted several times already, communication is essential and will allow you to learn about patient responses to such medications. Transport may need to be delayed until clinical stability is confirmed after medication administration.
ERROR TRAP #5: Failure to Execute the Plan Effectively as a Team
While transport of critically ill pediatric patients between hospitals is undertaken by specifically trained teams with specialized equipment, protocols, and standardized handoff procedures, intrahospital transport of comparably ill patients often occurs with ad hoc teams who are unfamiliar with each other (yet are expected to function effectively in a high stakes and time-sensitive environment), and involves variable degrees of organization and planning. Thinking about (and training in) teamwork as a distinct skill can help teach behaviors including effective leadership and followership, the shared mental model, identifying roles and responsibilities, and closed-loop communication. A pre-transport timeout should ideally occur and involve reviewing a transport checklist, agreeing upon roles and responsibilities, and establishing a shared mental model.
Individual and team-based training specific to transport among anesthesiologists is an understudied area. The ability to effectively lead a transport team in a resource-limited setting, such as an elevator or basement hallway, is a required skill for all pediatric anesthesiologists and one that could be honed with routine in situ simulation to identify latent safety threats, improve team performance, and promote competency in management of potential transport related adverse events. We hope that in the future there will be effective training for all of us in these areas.
How do you mitigate the risks of complex intrahospital transports and avoid these error traps? Should we focus more effort on educating our trainees (and ourselves) in management of transport complications? How do we continue to be proactive in efforts to increase transport safety as patient acuity, production pressure, and care volume continue to increase? Send your thoughts and comments to Myron (myasterster@gmail.com) who will post in a Friday Reader Response.
REFERENCES
1. Haydar B: Error Traps in the Intrahospital Transport of Critically Ill and Anesthetized Children. Paediatr Anaesth 2025; 35: 497–503.
2. Papson J, Russell K, Taylor D: Unexpected events during the intrahospital transport of critically ill patients. Acad Emerg Med 2007; 14: 574 – 577.
3. Murata M, Nakagawa N, Kawasaki T, Yasuo S, Yoshida T, Ando K, Okamori S, Okada Y: Adverse events during intrahospital transport of critically ill patients: A systematic review and meta-analysis. Am J Emerg Med 2022; 52 :13–19.
4. Nonami S, Kawakami D, Ito J, Ouchi K, Miyoshi Y, Tatebe M, Tsuchida T, Seo R, Mima H: Incidence of Adverse Events Associated With the In-Hospital Transport of Critically Ill Patients. Crit Care Explor 2022; 4:e0657.
5. Haydar B, Baetzel A, Stewart M, Voepel-Lewis T, Malviya S, and Christensen R: Complications Associated With the Anesthesia Transport of Pediatric Patients: An Analysis of the Wake Up Safe Database. Anesth Analg 2020; 131: 245 – 254.
6. Kohn L, Corrigan J, Donaldson M: Institute of Medicine (IOM) Report: To Err is Human: Building a Safer Health System., National Academy of Sciences, 1999.
7. Haydar B, Baetzel A, Elliott A, MacEachern M, Kamal A, Christensen R: Adverse Events During Intrahospital Transport of Critically Ill Children: A Systematic Review. Anesth Analg 2020; 131: 1135–1145.
8. Cooper JB, Lane-Fall MB: Anesthesia Needs to Lead the Way in Safety-Again-through the Universal Adoption of Structured Handoffs. Anesthesiology 2024; 140: 355–357.