I hope that over the past 3 weeks I’ve convinced many of you that intraoperative EEG monitoring to guide the administration of sevoflurane and propofol will become as common as pulse oximetry in all of our operating rooms. Instead of ‘flying blind”, intraoperative EEG can prevent under- and over-dosing by measuring the depth of hypnosis (unconsciousness) via changes in frequency, power, and other parameters of cortical electrical activity. Unlike pulse oximetry, which did not require any training to use, EEG monitoring will! How to implement this technology into your practice so that everyone in the anesthesia care team, attendings, residents, fellows, CRNAs, AAs, and students, can use it, regardless of patient age, is the goal of today’s Pediatric Anesthesia Article of the Day. I’ve asked Ian Yuan, Richard Missett, and Dean Kurth, authors of today’s paper, to help me in this review. I’ve also asked the leadership of the Society for Pediatric Anesthesia’s Education committee to consider having this topic discussed at an upcoming SPA annual conference. Myron Yaster MD
Original article
Yuan I, Missett RM, Jones-Oguh S, Massa CB, Babus LW, Garcia-Marcinkiewicz AG, Daly Guris RJ, Johnson G, McClung-Pasqualino H, Sequera-Ramos L, Iyer RS, Kurth CD. Implementation of an electroencephalogram-guided propofol anesthesia education program in an academic pediatric anesthesia practice. Paediatr Anaesth. 2022 Jul 6. doi: 10.1111/pan.14520. PMID: 35793171
“This QI education project implemented a standardized EEG TIVA training program over 12 months” at a single institution—the Children’s Hospital of Philadelphia. The program was assessed for effectiveness (significant improvement in EEG knowledge scores), scalability (training 50% of the staff), and sustainability (recurring EEG lectures for 80% of rotating residents and all new fellows and staff). The training program used the SedLine EEG monitor (Masimo Inc.), which displays 4 channel EEG waveforms, SEF (Spectral Edge Frequency), and DSA(Density Spectral Array); an infusion pump (Alaris Inc,) that delivers propofol in mg/kg (bolus) or μg/kg/min (infusion); and a modified electronic anesthesia record (EPIC) with a built-in propofol dosing table and reminders to enter SEF every 15 mintues.1
The key drivers and interventions included teaching content development (lectures, articles, and hand-outs), training a cohort of EEG TIVA teachers, intraoperative teaching (teaching points and dosing tables), decision support tools (dosing algorithms and anesthesia electronic record reminders), and testing knowledge (pre- and post-training examinations and intra-op verbal quizes)”.1
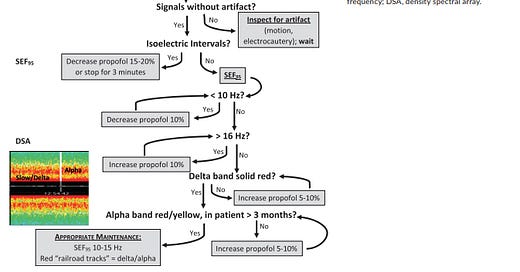
The teaching content focused on propofol PK/PD and using EEG parameters to titrate propofol to the desired anesthetic depth (figure). The key to their implementation success was the “teacher-learner-teacher paradigm. The learner, after completing EEG-TIVA training and intraoperative certification of knowledge and skill by the teacher, became a teacher for the next cohort of learners”.1 They also used intraoperative decision support algorithms for induction, maintenance and emergence. These decision-tree flowcharts provided learners a visual representation of how to use raw EEG, SEF, and DSA, to assess depth of hypnosis and titrate propofol dose to the desired effect site concentrations (Ce).2 Propofol Ce 4.5 μg/mL produces SEF 8–12 Hz, no beta power, and more delta than alpha power. Propofol Ce 3.0 μg/mL produces SEF 13–16 Hz, more alpha than delta and beta power.2 Propofol Ce 2.0 μg/mL produces beta and alpha power in addition to delta power.2
At the end of the training program, 80% of the staff were trained and certified in EEG-guided propofol TIVA, with significant improvement in EEG knowledge. The program continues to train the next cohort of new fellows and staff.
References
1. Yuan I, Missett RM, Jones-Oguh S, et al. Implementation of an electroencephalogram-guided propofol anesthesia education program in an academic pediatric anesthesia practice. Paediatric anaesthesia. Jul 6 2022;doi:10.1111/pan.14520
2. Xu T, Kurth CD, Yuan I, Vutskits L, Zhu T. An approach to using pharmacokinetics and electroencephalography for propofol anesthesia for surgery in infants. Paediatric anaesthesia. Dec 2020;30(12):1299-1307. doi:10.1111/pan.14021